[ad#superworm]
Veterinarians and veterinary technicians are often compared to pediatricians because our patients, like many of theirs, can’t tell us what is wrong. It takes a lot of education and long hours before we learn to recognize most of the things that can make your little critter sick. Even then it is a tough job. We only see patients once or twice a year. Sometimes it is difficult to tell if the way they are acting or feeling is normal for them. We just don’t see them enough. And when we ask what’s wrong, well, who knows what they would say if they could talk? This is where you, the owner, come in. One thing I have learned over the years is how important it is to listen to what you think is wrong with your pet. Because of the strong bonds and incredibly intimate relationships you share with your companions, you are often better at recognizing a potential medical problem than your veterinarian is. When it comes to what your pet is feeling, you are an expert.
[ad#sponsor]
When to Anesthetize
Anesthesia and analgesia are important specialties in reptile medicine that need further studies to determine effective drugs and dosage regimen. Along with the advances of diagnostic and surgical procedures in reptile medicine, safe and effective anesthetic techniques including appropriate pain relief therapy are required. This article describes clinical anesthetic techniques in reptiles.
When you bring your reptile to the vet for a problem or a procedure, the vet will need to determine the need for anesthesia or pain relief and the best method to administer it. Chemical restraint is often necessary in reptile medicine to facilitate procedures, from extracting the head of a leopard tortoise or box turtle from its shell simply to enable a blood sample to be obtained from its neck, to invasive procedures such as surgical correction of egg binding.
Before any anesthetic or sedative is administered, an assessment of the reptile patient’s health is necessary. Is sedation or anesthesia necessary for the procedure required? Is the reptile suffering from respiratory disease, or septicemia, hence is the reptile’s health likely to be made worse by sedation or anesthesia?
Injectable Anesthetics
Advantages of injectable anesthetics include ease of administration, avoiding breath holding and prolonged induction, low cost and availability. Disadvantages include a recovery often dependent on organ metabolism, potential difficulty reversing medications in emergency situations, and prolonged recovery periods, as well as degeneration of muscle cells at injection sites. Also, drugs injected into the upper half of a reptile may either be excreted by the kidneys before they take effect, or cause renal damage if they are toxic to the kidneys. Injectable medications should therefore be administered in the lower half of the body. Meditomadine and Ketamine are a good drug combination and are recommended in anesthetic protocol for most lizards as the “drug cocktail of choice.”
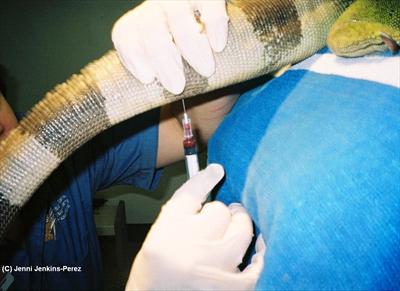
Reptiles generally receive injections through the tail vein. In most reptiles, intramuscular administration of anesthetic agents is most effective and practical. Although oral administration of sedative agents has been accomplished, this route of drug administration is not reliable. In snakes, intramuscular injections are given in the muscles next to the spine. Intravenous injections can be given in the jugular vein, or the tail vein. Most reptiles behave well for injections, however some, such as geckos, that are susceptible to autotomy, the act of an animal severing one or more of its own appendages, are at risk for dropping their tail.
Inhalant Anesthetics
Modern inhalant anesthetics such as halothane, isoflurane or sevoflurane can be used with oxygen or oxygen-nitrous oxide mixture in reptiles. Combining the inhalant anesthetic with nitrous oxide reduces the amount of inhalant required. Nitrous oxide used as an anesthetic adjunct is rapidly absorbed into the reptile‘s circulatory system, carrying the inhalant with it and speeding the induction time. It is rapidly exhaled through the lungs, shortening the time for recovery. Halothane and isoflurane are commonly used for anesthesia in many anesthesia species, including reptiles. Isoflurane is the inhalant anesthetic of choice because it has a lower blood/gas solubility compared with halothane, resulting in shorter induction and recovery periods. Sevoflurane, a newer inhalant with lower blood/gas solubility than isoflurane has been experimentally used in tortoises with good results. It has the potential to replace isoflurane in reptile anesthesia in the future.
Most inhalation agents can be administered for both induction of anesthesia and maintenance of anesthesia in reptiles. These anesthetics are administered through a mask that is placed over the reptile’s nose and mouth. Techniques for induction of anesthesia depend on the species, the procedure, and the health status of the patient. All reptiles need assisted breathing during anesthesia, so a tube will be placed once the animal is sedated. Through recovery, supplemental oxygen and heat is provided until the patient starts exhibiting normal reflexes such as eye and limb movements. Reptiles recovering from anesthesia should be monitored closely for distress or pain.
Safe and effective anesthesia can be challenging in reptiles because of their unique anatomy and physiology and their variable response to anesthetic and analgesic drugs and dosages. Commonly used anesthetic and analgesic agents may also be unpredictable and compromise stability of the reptilian patient. For successful anesthesia of the variety of reptilian species commonly seen by the veterinarian and veterinary technician, a thorough knowledge and understanding of their unique anatomy, physiology, and the pathophysiology of diseases is essential.


Great Article! I have been wondering how anaesthetic is administered.
What type of analgesic’s are there available for leopard gecko’s?
My leo recently underwent massive surgery for impaction, and she is in pain. Because she is in pain, she struggles when I have to force feed her. If there are any types of pain killers I can give her until she heals a bit more that would be great, as her struggling would harm her wound.
Also, is there anything I can buy over the counter to give her?
My leopard Geko had surgery to flush out an infection yesterday he is still really groggy and I’m worried ! How long do they take to wear off from anasetics ? Should I take him bk to vet if he’s not rite by saturday ?
I REALY WANT TO KNOW THE SAFEST ANESTHETIC AGENT USED FOR SNAKES